-
June
-
Renewable energy
-
Infotainment
-
Giro d'Italia
-
The Origin of Species
-
Eurovision Song Contest
-
Ignaz Semmelweis
-
Chocolate
-
Bouncer
-
Dante Alighieri
-
Anti-globalization movement
-
E-learning
-
Mad magazine
-
Dubai
-
Common English usage misconceptions
-
Logistics
-
Blue Is the Warmest Colour
-
Central Intelligence Agency (CIA)
-
Look-alike
-
Seigniorage
-
Reality television
-
Rihanna
-
Potential superpowers
-
Wicca
-
Musical instrument
-
Spelling bee
-
Stefano Rodotà
-
English Heritage
-
Singing
-
Femicide
|
WIKIMAG n. 7 - Giugno 2013
Ignaz Semmelweis
Text is available under the
Creative Commons Attribution-ShareAlike License; additional
terms may apply. See
Terms of
Use for details.
Wikipedia® is a registered trademark of the
Wikimedia Foundation,
Inc., a non-profit organization.
Traduzione
interattiva on/off
- Togli il segno di spunta per disattivarla

Ignaz Philipp Semmelweis[Note
1] (July 1, 1818 – August 13, 1865) (born Ignác Fülöp
Semmelweis) was a Hungarian physician of German extraction.[1]
[2]
now known as an early pioneer of antiseptic procedures. Described as the
"savior of mothers",[3]
Semmelweis discovered that the
incidence of
puerperal fever could be drastically cut by the use of hand
disinfection in
obstetrical clinics.[3]
Puerperal fever was common in mid-19th-century hospitals and often
fatal, with mortality at 10%–35%. Semmelweis postulated the theory of
washing with
chlorinated lime solutions in 1847[3]
while working in
Vienna General Hospital's First Obstetrical Clinic, where doctors'
wards had three times the mortality of
midwives' wards. He published a book of his findings in
Etiology, Concept and Prophylaxis of Childbed Fever.
Despite various publications of results where hand-washing reduced
mortality
to below 1%, Semmelweis's observations conflicted with the established
scientific and medical opinions of the time and his ideas were rejected
by the medical community. Some doctors were offended at the suggestion
that they should wash their hands and Semmelweis could offer no
acceptable scientific explanation for his findings. Semmelweis's
practice earned widespread acceptance only years after his death, when
Louis Pasteur confirmed the
germ theory and
Joseph Lister, acting on the French
microbiologist's research, practiced and operated, using hygienic
methods, with great success. In 1865, Semmelweis was committed to an
asylum, where he died at age 47 after being beaten by the guards,
only 14 days after he was committed.
Family and
early life

Teresia Müller and Josef Semmelweis, the parents of Ignaz
Semmelweis

Ignaz Semmelweis as a child in 1830
Ignaz Semmelweis was born on July 1, 1818 in the
Tabán, an
area of Buda,
part of present
Budapest, Hungary (then part of the
Austrian Empire). He was the fifth child out of ten of a prosperous
grocer
family of Josef and Teresia Müller Semmelweis.
His father, Josef Semmelweis (1778–1846), was born in
Kismarton, then part of Hungary, now
Eisenstadt, Austria. Josef achieved permission to set up shop in
Buda in 1806[Note
2] and, in the same year, opened a wholesale business with
spices and general consumer goods[Note
3] named zum Weißen Elefanten (at the White Elephant)
in Meindl-Haus in
Tabán
(today's 1-3, Apród Street, Semmelweis Museum of Medical History).[4]
By 1810, he was a wealthy man when he married Teresia Müller, daughter
of the famous coach (vehicle) builder Fülöp Müller.[5]
Ignaz Semmelweis began studying law at the
University of Vienna in the autumn of 1837, but by the following
year, for reasons that are no longer known, he had switched to medicine.
He was awarded his doctorate degree in medicine in 1844. After failing
to obtain an appointment in a clinic for internal medicine, Semmelweis
decided to specialize in obstetrics.[6]:16
Some of his teachers included
Carl von Rokitansky,
Josef Skoda and
Ferdinand von Hebra.
Discovery of cadaverous poisoning
Semmelweis was appointed assistant to Professor
Johann Klein in the First Obstetrical Clinic of the
Vienna General Hospital on July 1, 1846.[7]:72[Note
4] A comparable position today in a US hospital would be
"chief resident."[8]:56
His duties were to examine patients each morning in preparation for the
professor's rounds, supervise difficult deliveries, teach students of
obstetrics and be 'clerk' of records.
Maternity institutions were set up all over Europe to address
problems of
infanticide of illegitimate children. They were set up as gratis
institutions and offered to care for the infants, which made them
attractive to underprivileged women, including prostitutes. In return
for the free services, the women would be subjects for the training of
doctors and midwives. There were two maternity clinics at the Viennese
hospital. The First Clinic had an average
maternal
mortality rate due to puerperal fever of about 10% (actual
rates fluctuated wildly). The Second Clinic's rate was
considerably lower, averaging less than 4%. This fact was known outside
the hospital. The two clinics admitted on alternate days but women
begged to be admitted to the Second Clinic, due to the bad reputation of
the First Clinic.[6]:69
Semmelweis described desperate women begging on their knees not to be
admitted to the First Clinic.[6]:70
Some women even preferred to give birth in the streets, pretending to
have given sudden birth en route to the hospital (a practice
known as street births), which meant they would still qualify for
the child care benefits without having been admitted to the clinic.
Semmelweis was puzzled that puerperal fever was rare among women giving
street births. "To me, it appeared logical that patients who experienced
street births would become ill at least as frequently as those who
delivered in the clinic. [...] What protected those who delivered
outside the clinic from these destructive unknown endemic influences?"[6]:81
Semmelweis was severely troubled that his First Clinic had a much
higher mortality rate due to puerperal fever than the Second Clinic. It
"made me so miserable that life seemed worthless".[6]:86
The two clinics used almost the same techniques, and Semmelweis started
a meticulous process of eliminating all possible differences, including
even religious practices. The only major difference was the individuals
who worked there. The First Clinic was the teaching service for medical
students, while the Second Clinic had been selected in 1841 for the
instruction of midwives only.

Puerperal fever mortality rates for the First and Second
Clinic at the Vienna General Hospital 1841–1846. The First
Clinic evidently has the larger mortality rate.
Puerperal fever mortality rates for the First and Second Clinic
at the Vienna General Hospital 1841–1846. (Data
for more years are available.)
| |
First
clinic |
|
Second
clinic |
| Year |
Births |
Deaths |
Rate (%) |
|
Births |
Deaths |
Rate (%) |
| 1841 |
3,036 |
237 |
7.8 |
|
2,442 |
86 |
3.5 |
| 1842 |
3,287 |
518 |
15.8 |
|
2,659 |
202 |
7.6 |
| 1843 |
3,060 |
274 |
9.0 |
|
2,739 |
164 |
6.0 |
| 1844 |
3,157 |
260 |
8.2 |
|
2,956 |
68 |
2.3 |
| 1845 |
3,492 |
241 |
6.9 |
|
3,241 |
66 |
2.0 |
| 1846 |
4,010 |
459 |
11.4 |
|
3,754 |
105 |
2.8 |
He excluded "overcrowding" as a cause, since the Second Clinic was
always more crowded and yet the mortality was lower. He eliminated
climate as a cause because the climate was the same. The breakthrough
occurred in 1847, following the death of his good friend
Jakob Kolletschka, who had been accidentally poked with a student's
scalpel while performing a
postmortem examination. Kolletschka's own
autopsy
showed a
pathology similar to that of the women who were dying from puerperal
fever. Semmelweis immediately proposed a connection between
cadaveric
contamination and puerperal fever.
He concluded that he and the medical students carried "cadaverous
particles" on their hands[Note
5] from the autopsy room to the patients they examined in the
First Obstetrical Clinic. This explained why the student
midwives in the Second Clinic, who were not engaged in autopsies and
had no contact with corpses, saw a much lower mortality rate.
The
germ theory of disease had not yet been developed. Thus, Semmelweis
concluded some unknown "cadaverous material" caused childbed fever. He
instituted a policy of using a solution of
chlorinated lime (modern
calcium hypochlorite, the compound used in today's common household
chlorine bleach solution) for washing hands between autopsy work and the
examination of patients. He did this because he found that this
chlorinated solution worked best to remove the putrid smell of infected
autopsy tissue, and thus perhaps destroying the causal "poisonous" or
contaminating "cadaveric" agent hypothetically being transmitted by this
material.
The result was that the mortality rate in the First Clinic dropped
90%, and was then comparable to that in the Second Clinic. The mortality
rate in April 1847 was 18.3%. After hand washing was instituted in
mid-May, the rates in June were 2.2%, July 1.2%, August 1.9% and, for
the first time since the introduction of anatomical orientation, the
death rate was zero in two months in the year following this discovery.
Efforts to reduce childbed fever
Semmelweis demonstrated that puerperal fever (also known as childbed
fever) was contagious and that this incidence could drastically be
reduced by appropriate hand washing by medical care-givers. He made this
discovery in 1847 while working in the Maternity Department of the
Vienna Lying-in Hospital. His failure to convince his fellow doctors led
to a tragic conclusion, however, he was ultimately vindicated and
cleared of blame. While employed as assistant to the professor of the
maternity clinic at the
Vienna General Hospital in
Austria
in 1847, Semmelweis introduced hand washing with
chlorinated lime solutions for interns who had performed autopsies.
This immediately reduced the incidence of fatal puerperal fever from
about 10 percent (range 5–30 percent) to about 1–2 percent. At the time,
diseases were attributed to many different and unrelated causes. Each
case was considered unique, just as a human person is unique.
Semmelweis's hypothesis, that there was only one cause, that all that
mattered was cleanliness, was extreme at the time, and was largely
ignored, rejected or ridiculed. He was dismissed from the hospital for
political reasons and harassed by the medical community in Vienna, being
eventually forced to move to Budapest.
Semmelweis was outraged by the indifference of the medical profession
and began writing open and increasingly angry letters to prominent
European obstetricians, at times denouncing them as irresponsible
murderers. His contemporaries, including his wife, believed he was
losing his mind, and in 1865 he was committed to an
asylum. In an ironic twist of fate, he died there of
septicaemia only 14 days later, possibly as the result of being
severely beaten by guards. Semmelweis's practice earned widespread
acceptance only years after his death, when
Louis Pasteur developed the
germ theory of disease, offering a theoretical explanation for
Semmelweis's findings. He is considered a pioneer of antiseptic
procedures.
Conflict with established medical opinions

Puerperal fever monthly mortality rates for the First
Clinic at Vienna Maternity Institution 1841–1849. Rates drop
markedly when Semmelweis implemented chlorine hand washing
mid-May 1847
(see rates).
Semmelweis's observations conflicted with the established scientific
and medical opinions of the time. The theory of
diseases
was highly influenced by ideas of an imbalance of the basic "four
humours" in the body, a theory known as
dyscrasia, for which the main treatment was
bloodlettings. Medical texts at the time emphasized that each case
of disease was unique, the result of a personal imbalance, and the main
difficulty of the medical profession was to establish precisely each
patient's unique situation, case by case.
The findings from autopsies of deceased women also showed a confusing
multitude of physical signs, which emphasized the belief that puerperal
fever was not one, but many different, yet unidentified, diseases.
Semmelweis's main finding — that all instances of puerperal fever could
be traced back to only one single cause: lack of cleanliness — was
simply unacceptable. His findings also ran against the conventional
wisdom that diseases spread in the form of "bad air", also known as
miasmas or vaguely as "unfavourable atmospheric-cosmic-terrestrial
influences". Semmelweis's groundbreaking idea was contrary to all
established medical understanding.
As a result, his ideas were rejected by the medical community. Other
more subtle factors may also have played a role. Some doctors, for
instance, were offended at the suggestion that they should wash their
hands, feeling that their social status as gentlemen was inconsistent
with the idea that their hands could be unclean.[8]:9[Note
6]
Specifically, Semmelweis's claims were thought to lack scientific
basis, since he could offer no acceptable explanation for his findings.
Such a scientific explanation was made possible only some decades later,
when the
germ theory of disease was developed by
Louis Pasteur,
Joseph Lister, and others.
During 1848, Semmelweis widened the scope of his washing protocol, to
include all instruments coming in contact with patients in labour, and
used mortality rates
time series to document his success in virtually eliminating
puerperal fever from the hospital ward.
Hesitant publication of results and first signs of trouble
Toward the end of 1847, accounts of Semmelweis's work began to spread
around Europe. Semmelweis and his students wrote letters to the
directors of several prominent maternity clinics describing their recent
observations.
Ferdinand von Hebra, the editor of a leading Austrian medical
journal, announced Semmelweis's discovery in the December 1847[9]
and April 1848[10]
issues of the medical journal. Hebra claimed that Semmelweis's work had
a practical significance comparable to that of
Edward Jenner's introduction of cowpox inoculations to prevent
smallpox.[8]:54–55
In late 1848, one of Semmelweis's former students wrote a lecture
explaining Semmelweis's work. The lecture was presented before the Royal
Medical and Surgical Society in London and a review published in
The
Lancet, a prominent medical journal.[Note
7] A few months later, another of Semmelweis's former students
published a similar essay in a French periodical.[11]
As accounts of the dramatic reduction in mortality rates in Vienna
were being circulated throughout Europe, Semmelweis had reason to expect
that the chlorine washings would be widely adopted, saving tens of
thousands of lives. Early responses to his work also gave clear signs of
coming trouble, however. Some physicians had clearly misinterpreted his
claims.
James Young Simpson, for instance, saw no difference between
Semmelweis's groundbreaking findings and the British idea suggested by
Oliver Wendell Holmes in 1843 that childbed fever was contagious
(i.e. that infected persons could pass the infection to others).[6]:10–12*
Indeed, initial responses to Semmelweis's findings were that he had
said nothing new.[6]:31*
In fact, Semmelweis was warning against all decaying organic matter,
not just against a specific contagion that originated from victims of
childbed fever themselves. This misunderstanding, and others like it,
occurred partly because Semmelweis's work was known only through
secondhand reports written by his colleagues and students. At this
crucial stage, Semmelweis himself had published nothing. These and
similar misinterpretations would continue to cloud discussions of his
work throughout the century.[8]:56
Some accounts emphasize that Semmelweis refused to communicate his
method officially to the learned circles of Vienna,[12]:37
nor was he eager to explain it on paper.
Political turmoil and dismissal from the Vienna hospital
In 1848
a series of tumultuous revolutions swept across Europe. The
resulting political turmoil would affect Semmelweis's career. In Vienna
on March 13, 1848, students demonstrated in favor of increased civil
rights, including trial by jury and freedom of expression. The
demonstrations were led by medical students and young faculty members
and were joined by workers from the suburbs. Two days later in Hungary,
demonstrations and uprisings led to the
Hungarian Revolution of 1848 and a full-scale war against the ruling
Habsburgs of the
Austrian Empire. In Vienna, the March demonstration was followed by
months of general unrest.[8]:57
There is no evidence that Semmelweis was personally involved in the
events of 1848. It is known that some of his brothers were punished for
active participation in the Hungarian independence movement, and it
seems likely that the Hungarian-born Semmelweis was sympathetic to the
cause. Semmelweis's superior, professor
Johann Klein, was a conservative Austrian, likely uneasy with the
independence movements and alarmed by the other
revolutions of 1848 in the Habsburg areas. It seems likely that
Klein mistrusted Semmelweis.[8]:59
When Semmelweis's term was about to expire
Carl Braun also applied for the position of assistant in the
First Clinic, possibly at Klein's own invitation. Semmelweis and Braun
were the only two applicants for the post. Semmelweis's predecessor,
Breit, had been granted a two-year extension.[6]:61,
105 Semmelweis's application for an extension was supported by
Josef Škoda and
Carl von Rokitansky and by most of the medical faculty, but Klein
chose Braun for the position. Semmelweis was obliged to leave the
obstetrical clinic when his term expired on March 20, 1849.[8]:61
The day his term expired, Semmelweis petitioned the Viennese
authorities to be made
docent of obstetrics. A docent was a private lecturer who taught
students and who had access to some university facilities. At first,
because of Klein's opposition, Semmelweis's petition was denied. He
reapplied, but had to wait until October 10, 1850 (more than 18 months)
before finally being appointed docent of theoretical obstetrics.[6]:105
The terms refused him access to cadavers and limited him to teaching
students by using leather-fabricated
mannequins only. A few days after being notified of his appointment,
Semmelweis left Vienna abruptly and returned to Pest. It appears that he
left without so much as saying good-bye to his former friends and
colleagues, a move that may have offended them.[6]:52
According to his own account, he left Vienna because he was "unable to
endure further frustrations in dealing with the Viennese medical
establishment".[8]:67
Life in Budapest

Wedding portraits of Ignaz Semmelweis and Maria Weidenhoffer
(1857)
During 1848–1849 some 70 000 troops from
the
Habsburg-ruled
Austrian Empire thwarted the
Hungarian independence movement, executed or imprisoned its leaders
and in the process destroyed parts of
Pest. It seems likely that Semmelweis, upon arriving from the
Habsburg Vienna in 1850, was not warmly welcomed in Pest.
On May 20, 1851 Semmelweis took the relatively insignificant, unpaid,
honorary head-physician position of the obstetric ward of Pest's small
St. Rochus Hospital. He held that position for six years, until June
1857.[6]:107[8]:68
Childbed fever was rampant at the clinic; at a visit in 1850, just after
returning to Pest, Semmelweis found one fresh corpse, another patient in
severe agony, and four others seriously ill with the disease. After
taking over in 1851, Semmelweis virtually eliminated the disease. During
1851–1855 only 8 patients died from childbed fever out of 933 births
(0.85%).[6]:106–108
Despite the impressive results, Semmelweis's ideas were not accepted
by the other obstetricians in Budapest.[8]:69
The professor of obstetrics at the University of Pest,
Ede Flórián Birly, never adopted Semmelweis's methods. He continued
to believe that puerperal fever was due to uncleanliness of the bowel.[6]:24*
Therefore, extensive purging was the preferred treatment.
After Birly died in 1854, Semmelweis applied for the position. So did
Carl Braun — Semmelweis's nemesis and successor as
Johann Klein's assistant in Vienna — and Braun received more votes
from his Hungarian colleagues than Semmelweis did. Semmelweis was
eventually appointed in 1855, but only because the Viennese authorities
overruled the wishes of the Hungarians, as Braun did not speak
Hungarian. As professor of obstetrics, Semmelweis instituted chlorine
washings at the University of Pest maternity clinic. Once again, the
results were impressive.[8]:69
Semmelweis declined an offer in 1857 to become professor of
obstetrics at the
University of Zurich.[6]:56
The same year, Semmelweis married Maria Weidenhoffer (1837–1910),
nineteen years his junior and the daughter of a successful merchant in
Pest. They had five children: a son who died shortly after birth, a
daughter who died at the age of 4 months, another son who committed
suicide at age 23 (possibly due to gambling debts), another daughter who
would remain unmarried, and a third daughter who would have children of
her own.[8]:70

Semmelweis's main work: Die Ätiologie, der Begriff und
die Prophylaxis des Kindbettfiebers, 1861 (front page)
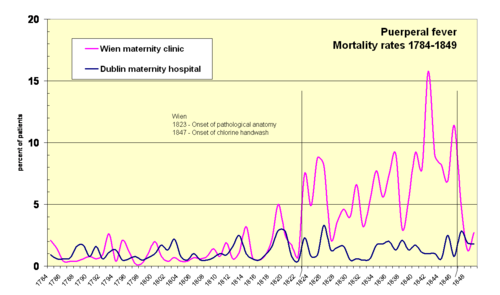
In his 1861 book, Semmelweis presented evidence to
demonstrate that the advent of
pathological anatomy in Wien (Vienna) in 1823 (vertical
line) was accompanied by the increased incidence of fatal
childbed fever. The second vertical line marks introduction
of chlorine hand washing in 1847. Rates for the Dublin
maternity hospital, which had no pathological anatomy, are
shown for comparison ( view
rates).
One of the first to respond to Semmelweis's 1848 communications was
James Young Simpson who wrote a stinging letter. Simpson surmised
that the English obstetrical literature must be totally unknown in
Vienna, or Semmelweis would have known that the English had long
regarded childbed fever as contagious and would have employed chlorine
washing to protect against it.[6]:174
Semmelweis's views were much more favorably received in England than
on the continent, but he was more often cited than understood. The
English consistently regarded Semmelweis as having supported their
theory of contagion. A typical example was W. Tyler Smith, who claimed
that Semmelweis "made out very conclusively" that "miasms
derived from the dissecting room will excite puerperal disease."[6]:176*[13]:504
In 1856, Semmelweis's assistant Josef Fleischer reported the
successful results of handwashings at St. Rochus and Pest maternity
institutions in the Viennese Medical Weekly (Wiener
Medizinische Wochenschrift).[8]:69
The editor remarked sarcastically that it was time people stopped being
misled about the theory of chlorine washings.[6]:24[14]:536
In 1858 Semmelweis finally published his own account of his work in
an essay entitled, "The Etiology of Childbed Fever".[Note
8] Two years later he published a second essay, "The
Difference in Opinion between Myself and the English Physicians
regarding Childbed Fever".[Note
9] In 1861, Semmelweis finally published his main work Die
Ätiologie, der Begriff und die Prophylaxis des Kindbettfiebers
(German for The Etiology, Concept and Prophylaxis of Childbed Fever).
In his 1861 book, Semmelweis lamented the slow adoption of his ideas:
"Most medical lecture halls continue to resound with lectures on
epidemic childbed fever and with discourses against my theories. […] The
medical literature for the last twelve years continues to swell with
reports of puerperal epidemics, and in 1854 in Vienna, the birthplace of
my theory, 400 maternity patients died from childbed fever. In published
medical works my teachings are either ignored or attacked. The medical
faculty at Würzburg awarded a prize to a monograph written in 1859 in
which my teachings were rejected".[6]:169[Note
10]
In Berlin, the professor of obstetrics,
Joseph Hermann Schmidt, approved of obstetrical students having
ready access to morgues in which they could spend time while waiting for
the labor process.[6]:34[16]:501
In a textbook,
Carl Braun, Semmelweis's successor as assistant in the first clinic,
identified 30 causes of childbed fever; only the 28th of these was
cadaverous infection. Other causes included conception and pregnancy,
uremia, pressure exerted on adjacent organs by the shrinking uterus,
emotional traumata, mistakes in diet, chilling, and atmospheric epidemic
influences.[17][Note
11] The impact of Braun's views are clearly visible in the
rising mortality rates in the 1850s.
Ede Flórián Birly, Semmelweis's predecessor as Professor of
Obstetrics at the University of Pest, never accepted Semmelweis's
teachings; he continued to believe that puerperal fever was due to
uncleanliness of the bowel.[6]:4*
August Breisky, an obstetrician in Prague, rejected Semmelweis's
book as "naive" and he referred to it as "the Koran of puerperal
theology". Breisky objected that Semmelweis had not proved that
puerperal fever and
pyemia are identical, and he insisted that other factors beyond
decaying organic matter certainly had to be included in the
etiology of the disease.[6]:41[18]:1
Carl Edvard Marius Levy, head of the Copenhagen maternity hospital
and an outspoken critic of Semmelweis's ideas, had reservations
concerning the unspecific nature of cadaverous particles and that the
supposed quantities were unreasonably small. "If Dr. Semmelweis had
limited his opinion regarding infections from corpses to puerperal
corpses, I would have been less disposed to denial than I am. […]
And, with due respect for the cleanliness of the Viennese students, it
seems improbable that enough infective matter or vapor could be secluded
around the fingernails to kill a patient."[6]:180–181[19]
In fact,
Robert Koch later used precisely this fact to prove that various
infecting materials contained living organisms which could reproduce in
the human body, i.e. since the poison could be neither chemical
nor physical in operation, it must be biological.[6]:183*
At a conference of German physicians and
natural scientists, most of the speakers rejected his doctrine,
including the celebrated
Rudolf Virchow, who was a scientist of the highest authority of his
time. Virchow’s great authority in medical circles contributed potently
to the lack of recognition of the Semmelweis doctrine for a long time.[15]
It has been contended that Semmelweis could have had an even greater
impact if he had managed to communicate his findings more effectively
and avoid antagonising the medical establishment, even given the
opposition from entrenched viewpoints.[20]
Breakdown, death and oblivion

Semmelweis's 1862 Open Letter to all Professors of
Obstetrics
Beginning in 1861, Semmelweis suffered from various nervous
complaints. He suffered from severe depression and became excessively
absentminded. Paintings from 1857 to 1864 show a progression of aging.[Note
12] He turned every conversation to the topic of childbed
fever.
After a number of unfavorable foreign reviews of his 1861 book,
Semmelweis lashed out against his critics in a series of Open Letters.[Note
13] They were addressed to various prominent European
obstetricians, including
Späth,
Scanzoni,
Siebold, and to "all obstetricians". They were full of bitterness,
desperation, and fury and were "highly polemical and superlatively
offensive"[6]:57
at times denouncing his critics as irresponsible murderers[8]:73
or ignoramuses.[6]:41
He also called upon Siebold to arrange a meeting of German obstetricians
somewhere in Germany to provide a forum for discussions on puerperal
fever where he would stay "until all have been converted to his theory."[15]
In mid-1865, his public behaviour became irritating and embarrassing
to his associates. He also began to drink immoderately; he spent
progressively more time away from his family, sometimes in the company
of a prostitute; and his wife noticed changes in his sexual behavior. On
July 13, 1865 the Semmelweis family visited friends, and during the
visit Semmelweis's behavior seemed particularly inappropriate.[8]:74
The exact nature of Semmelweis’s affliction has been a subject of
some debate. According to K Codell Carter, in his biography of
Semmelweis, the exact nature of his affliction cannot be determined. “It
is impossible to appraise the nature of Semmelweis's disorder. It may
have been
learned helplessness, which is known to cause chronic and severe
depression. It may have been
Alzheimer's disease, a type of dementia, which is associated with
rapid cognitive decline and mood changes.[20]:270
It may have been third stage
syphilis, a then-common disease of obstetricians who examined
thousands of women at gratis institutions, or it may have been emotional
exhaustion from overwork and stress.”[8]:75
Investigative reporter Michael Volpe argued that Semmelweis was
suffering from a form of post-traumatic stress disorder (PTSD) and this
is what caused the erratic, confrontational, and repellant behavior that
Semmelweis exhibited, especially toward the end of his life.[21]
Volpe argued that the original source of Semmelweis’s trauma could have
been linked to a number of deaths including: all the women that were
dying at the First Obstetricianal clinic at Vienna General Hospital in
1846, his son Jakob Kolletschka, who died at childbirth, and his
colleague Gustav Adolph Michaelis, who killed himself because he blamed
himself for a death from childbed fever. That trauma was repeated
through Semmelweis’s many professional losses until he broke down.
Semmelweis’s drinking and visiting a prostitute would have been two
examples of avoidance behavior, standard in sufferers of PTSD.[21]
In 1865
János Balassa wrote a document referring Semmelweis to a mental
institution. On July 30
Ferdinand Ritter von Hebra lured him, under the pretense of visiting
one of Hebra's "new Institutes", to a Viennese insane asylum located in
Lazarettgasse (Landes-Irren-Anstalt in der Lazarettgasse).[7]:293
Semmelweis surmised what was happening and tried to leave. He was
severely beaten by several guards, secured in a
straitjacket and confined to a darkened cell. Apart from the
straitjacket, treatments at the
mental institution included dousing with cold water and
administering
castor oil, a
laxative. He died after two weeks, on August 13, 1865, aged 47, from
a
gangrenous wound, possibly caused by the beating. The autopsy
revealed extensive internal injuries, the cause of death
pyemia—blood
poisoning.[8]:76–78
Semmelweis was buried in Vienna on August 15, 1865. Only a few people
attended the service.[8]:78
Brief announcements of his death appeared in a few medical periodicals
in Vienna and Budapest. Although the rules of the Hungarian Association
of Physicians and Natural Scientists specified that a commemorative
address be delivered in honor of a member who had died in the preceding
year, there was no address for Semmelweis; his death was never even
mentioned.[8]:79
János Diescher was appointed Semmelweis's successor at the Pest
University maternity clinic. Immediately mortality rates jumped sixfold
to six percent. But the physicians of Budapest said nothing; there were
no inquiries and no protests. Almost no one — either in Vienna or in
Budapest — seems to have been willing to acknowledge Semmelweis's life
and work.[8]:79
His remains were transferred to Budapest in 1891. On October 11, 1964
they were transferred once more to the house in which he was born. The
house[22]
is now a historical museum and library, honoring Ignaz Semmelweis.[6]:58
Legacy

Microbial cultures demonstrating the effectiveness of
disinfection: without disinfection procedures (A), after
washing hands with soap (B) and after disinfection with
alcohol (C)
Semmelweis's advice on chlorine washings was probably more
influential than he realized himself. Many doctors, particularly in
Germany, appeared quite willing to experiment with the practical hand
washing measures that he proposed, but virtually everyone rejected his
basic and ground-breaking theoretical innovation—that the disease had
only one cause, lack of cleanliness.[6]:48
Professor
Gustav Adolf Michaelis from a maternity institution in
Kiel
replied positively to Semmelweis's suggestions—eventually he committed
suicide, however, because he felt responsible for the death of his own
cousin, whom he had examined after she gave birth.[6]:176–178
Only belatedly did his observational evidence gain wide acceptance;
more than twenty years later,
Louis Pasteur's work offered a theoretical explanation for
Semmelweis's observations—the
germ theory of disease. As such, the Semmelweis story is often used
in university courses with
epistemology content, e.g. philosophy of science
courses—demonstrating the virtues of
empiricism or
positivism and providing a historical account of which types of
knowledge count as scientific (and thus accepted) knowledge, and which
do not. It has been seen as an irony that Semmelweis's critics
considered themselves positivists, but even positivism suffers problems
in the face of theories which seem magical or superstitious, such as the
idea that "corpse particles" might turn a person into a corpse, with no
causal mechanism being stipulated, after a simple contact. They could
not accept Semmelweis' ideas of minuscule and largely invisible amounts
of decaying organic matter as a cause of every case of childbed fever—
ideas which in the absence of a replicative biological mechanism, must
have seemed no more chemically likely than
homeopathy. To his contemporaries, Semmelweis seemed to be reverting
to the speculative theories of earlier decades that were so repugnant to
his positivist contemporaries.[6]:45
The so-called
Semmelweis reflex — a metaphor for a certain type of human behaviour
characterized by reflex-like rejection of new knowledge because it
contradicts entrenched norms, beliefs or paradigms — is named after
Semmelweis, whose perfectly reasonable hand-washing suggestions were
ridiculed and rejected by his contemporaries.
Other legacies of Semmelweis include:
- Semmelweis is now recognized as a pioneer of
antiseptic policy
-
Semmelweis University, a university for medicine and
health-related disciplines (located in
Budapest, Hungary), is named after Semmelweis; and
- The Semmelweis Orvostörténeti Múzeum (Semmelweis Medical
History Museum) is located in the former home of Semmelweis[22]
- The Semmelweis Klinik, a hospital for women located in Vienna,
Austria
- The Semmelweis Hospital in
Miskolc, Hungary
- In 2008 Semmelweis was selected as the motif for an Austrian
commemorative coin.[23]
Film
Literature
-
Semmelweis, Ignác; von Györy, Tiberius (1905),
Semmelweis's Gesammelte Werke Herausgegeben und zum Theil aus dem
Ungarischen Übersetzt [The complete published works of
Semmelweis, in part published from Hungarian] (in German),
Jena Verlag von Gustav Fischer, p. 604
is the classic reference, in Latin print, not the original Gothic
print.
-
Louis-Ferdinand Céline completed his Ph. D. thesis on Semmelweis
in 1924. It was published as a fictionalized biography under the
title La Vie et l'œuvre de Philippe Ignace Semmelweis in 1936
(English: The Life and Work of Semmelweis, tr. by Robert
Allerton Parker, Boston : Little, Brown and Company, 1937/The
Life and Work of Semmelweiss: A Fictional Biography, tr. by John
Harman, Atlas Press, 2008).
-
Morton Thompson's 1949 novel
The Cry and the Covenant is a fictionalized account based on
the life of Semmelweiss.
Drama / Plays
- "Semmelweis" by Howard Sackler. Performed in 1977 at Studio
Arena Theater in Buffalo, NY with Lewis J. Stadlen, Kathy Bates, and
Kim Hunter. Performed in 1978 at Kennedy Center in Washington D.C.
with Colin Blakeley. Performed in 1981 at Hartman Theater in
Stamford, CT.
See also
Notes
-
^
The name "Semmelweis" is not
spelled with ss as in
weiss, but uses the shorter suffix -weis
(omits the second s), (significance: bread roll- or bun-white ).
Ignaz Semmelweis is pronounced, using typical Austrian (a
German-dialect) pronunciation rules, as "igg-nahts seml-vice" (w
is spoken like v).
-
^
translated from: [er] erhielt 1806
das Bürgerrecht in Buda[clarification
needed]
-
^
translated from: Spezereien- und
Kolonialwarengroßhandlung[clarification
needed]
-
^
Details: On July 1, 1844 Semmelweis
became a trainee physician's assistant at the Vienna maternity
clinic (in German, Aspirant Assistentarztes an der Wiener
Geburtshilflichen Klinik) and on July 1, 1846 he was
appointed an ordinary physician's assistant (in German,
ordentlicher Assistentarzt). However, on October 20, 1846
his predecessor Dr.
Franz Breit (an obstetrician) unexpectedly returned, and
Semmelweis was demoted. By March 20, 1847, Dr. Breit was
appointed professor in
Tübingen and Semmelweis resumed the Assistentarzt
position.[7]:72
-
^
Semmelweis's reference to
"cadaverous particles" were (in German) "an der Hand klebende
Cadavertheile"[7]:95
-
^
See for instance
Charles Delucena Meigs, in which there is a link to an
original source document.
-
^
The author of the lecture was
Charles Henry Felix Routh, but it was delivered by Edward
William Murphy since Routh was not a Fellow of the Royal Medical
and Surgical Society. (Lecture: On the Causes of the Endemic
Puerperal Fever of Vienna, Medico-chirurgical Transactions
32(1849): 27-40. Review: Lancet 2(1848): 642f.) For a list of
some other reviews, see Frank P. Murphy, "Ignaz Philipp
Semmelweis (1818–1865): An Annotated Bibliography," Bulletin of
the History of Medicine 20(1946), 653-707: 654f.[6]:175*
-
^
The report was "A gyermekágyi láz
kóroktana" ("The Etiology of Childbed Fever") published in
Orvosi hetilap 2 (1858); a translation into German is
included in Tiberius von Györy's, Semmelweis's gesammelte
Werke (Jena: Gustav Fischer, 1905), 61–83. This was
Semmelweis's first publication on the subject of puerperal
fever. According to Győry the substance of the report was
contained in lectures delivered before the Budapester
Königliche Ârzteverein in the spring of 1858.[6]:112*
-
^
The article was originally
published as: Ignaz Philipp Semmelweis, "A gyermekágyi láz
fölötti véleménykülönbség köztem s az angol orvosok közt" Orvosi
hetilap 4 (1860), 849–851, 873-76, 889–893, 913–915.[6]:24*
-
^
The monograph to which Semmelweis
refers was a work by Heinrich Silberschmidt,
"Historisch-kritische Darstellung der Pathologie des
Kindbettfiebers von den ältesten Zeiten bis auf die unserige",
published 1859 in
Erlangen, which mentions Semmelweis only incidentally and
without dealing at all with the transfer of toxic materials by
the hands of physicians and midwives. The book was awarded a
prize by the medical faculty of Würzburg at the instigation of
Friedrich Wilhelm Scanzoni von Lichtenfels[15][6]:212*
-
^
Carl Braun's thirty causes appear
in his Lehrbuch der Geburtshülfe. In the first of these,
published in 1855, he mentions Semmelweis in connection with his
discussion of cause number 28, cadaverous poisoning. In the
later version, however, although he discusses the same cause in
the same terms, all references to Semmelweis have been dropped.[6]:34*
-
^
Paintings of Semmelweis available
in the 1983 edition of his Etiology, Concept and Prophylaxis
of Childbed Fever,[6]:57
and at
Wikimedia Commons.
-
^
The 1862 open letter is available
at the
Austrian national library website.
References
-
^
"Ignaz Philipp Semmelweis". Semmelweis Society International.
Retrieved 28 May 2013.
-
^
Encyclopedia Britannica: Ignaz Philipp Semmelweis
- ^
a
b
c
Hanninen,
O.; Farago, M.; Monos, E. (September–October 1983),
"Ignaz Philipp Semmelweis, the prophet of bacteriology",
Infection Control 4 (5): 367–370,
PMID 6354955,
archived from
the original on April 4, 2008,
retrieved October 26, 2009, "Only the clinical facts
proved him right during his lifetime; the triumph of
bacteriology which began after his death made him not only the
"savior of mothers" but also a genial ancestor of bacteriology."
-
^
"Semmelweis Orvostörténeti Múzeum, Könyvtár és Levéltár -
Semmelweis Ignác - Élete". Semmelweis.museum.hu.
Retrieved 2012-05-19.
-
^
Antall, József; Szebellédy, Géza (1973), Aus den
Jahrhunderten der Heilkunde, Budapest: Corvina Verlag,
pp. 7–8
-
^
a
b
c
d
e
f
g
h
i
j
k
l
m
n
o
p
q
r
s
t
u
v
w
x
y
z
aa
ab
ac
ad
ae
af
ag
ah
ai
Semmelweis,
Ignaz; Carter, K. Codell (translator, extensive foreword)
(September 15, 1983) [1861], Etiology, Concept and
Prophylaxis of Childbed Fever, University of Wisconsin
Press,
ISBN 0-299-09364-6
(references to Carter's foreword and notes indicated "*")
- ^
a
b
c
d
Benedek, István
(1983), Ignaz Phillip Semmelweis 1818–1865, Druckerei
Kner, Gyomaendrőd, Hungary: Corvina Kiadó (Translated from
Hungarian to German by Brigitte Engel),
ISBN 963-13-1459-6
- ^
a
b
c
d
e
f
g
h
i
j
k
l
m
n
o
p
q
r
s
t
Carter, K.
Codell; Carter, Barbara R. (February 1, 2005), Childbed
fever. A scientific biography of Ignaz Semmelweis,
Transaction Publishers,
ISBN 978-1-4128-0467-7
-
^
Hebra, Ferdinand (1847), "Höchst wichtige Erfahrungen über
die Aetiologie der an Gebäranstalten epidemischen
Puerperalfieber", Zeitschrift der k.k. Gesellschaft der Ärzte
zu Wien 4 (1): 242–244
-
^
Hebra, Ferdinand (1848), "Fortsetzung der Erfahrungen über
die Aetiologie der in Gebäranstalten epidemischen
Puerperalfieber", Zeitschrift der k.k. Gesellschaft der Ärzte
zu Wien 5: 64f
-
^
Wieger, Friedrich
(1849), "Des moyens prophylactiques mis en U.S.A.ge au grand
hôpital de Vienne contre l'apparition de la fièvre puerpérale",
Gazette médicale de Strasbourg (in French) 9:
99–105
-
^
Reid, Robert William (1975), "Microbes and Men", Nature
(New York, NY, U.S.A.: Saturday Review Press) 251 (5472):
266,
Bibcode:1974Natur.251..266L,
doi:10.1038/251266a0,
ISBN 978-0-8415-0348-9,
OCLC 1227698
-
^
"Puerperal Fever",
The Lancet 2, 1856: 503–505
-
^
Fleischer, J.
(1856),
"Statistischer Bericht der Gebärklinik an der kk. Universität zu
Pest im Schuljahre 1855–56", Wiener medizinische
Wochenschrift (in German) 6: 534–536,
retrieved May 11, 2008, "Wir glaubten diese
Chlorwaschungs-Theorie habe sich längst überlebt; die
Erfahrungen und statistichen Ausweisse der meisten
geburtshilflichen Anstalten protestieren gegen ubige Anschanung;
es wäre an der Zeit sich von dieser Theorie nicht weiter
irreführen zu lassen."
- ^
a
b
c
Hauzman, Erik E.
(August 26–30, 2006),
"Semmelweis and his German contemporaries" (DOC),
40th International Congress on the History of Medicine, ISHM
2006, Budapest, Hungary,
retrieved March 24, 2009
-
^
Schmidt, Joseph Hermann (1850), "Die
geburtshülfliche-klinischen Institute der königlichen Charité",
Annalen des charité-Krankenhauses zu Berlin 1:
485–523
-
^
Braun, Carl (1857), Lehrbuch der Geburtshülfe,
Vienna, Austria: Braumüller
-
^
Breisky, August
(1861), Vierteljahrschrift fur die praktische Heilkunde 18
Literarischer Anzeiger 2: 1–13
-
^
Levy, Karl Edouard
Marius (1848), "De nyeste Forsög i Födselsstiftelsen i Wien til
Oplysning om Barselfeberens Aetiologie",
Hospitals-Meddelelser 1: 199–211
- ^
a
b
Nuland, Sherwin B. (2003), The Doctors' Plague: Germs,
Childbed Fever and the Strange Story of Ignac Semmelweis, W.
W. Norton,
ISBN 0-393-05299-0
- ^
a
b
Volpe,
Michael (2013). The Definitive Dossier of PTSD (Chapter 5).
Kindle.
-
^
a
b
"Semmelweis Orvostörténeti Múzeum website".
Semmelweis.museum.hu.
Retrieved 2012-05-19.
-
^
"50 Euro - Ignaz Philipp Semmelweis (2008)",
Austrian Mint website (Vienna), archived from
the original on October 27, 2009,
retrieved October 27, 2009, "The new gold coin with a
face value of 50 Euro has a portrait of the celebrated doctor
himself together with the staff of Aesculapius, which is the
logo for the entire series. The reverse has a bird’s-eye view of
the old General Hospital in Vienna, where Semmelweis was
stationed in the childbirth clinic. An insert to the right shows
a doctor and a student in the act of disinfecting their hands
before examining a patient."
External links
-
Sloan Science and Film / Short Films / Semmelweis by Jim Berry
17 minutes
- Extracts from Semmelweis's 1861 book, The Etiology, Concept, and
Prophylaxis of Childbed Fever were published in the January 2008
edition of
Social Medicine
-
BMJ: Ignaz Semmelweis
-
Catholic Encyclopedia entry
- John H. Lienhard (1991). "Ignaz
Philipp Semmelweis".
The Engines of Our Ingenuity. Episode 622. NPR. KUHF-FM
Houston.
-
Who Named it? Ignaz Philipp Semmelweis
-
Tan S Y and Brown J Ignaz Philipp Semmelweis
-
Caroline M De Costa, The contagiousness of childbed fever : a short
history of puerperal sepsis and its treatment, eMJA The Medical
Journal of Australia, MJA 2002 177 (11/12): 668–671
-
review, The Fool of Pest, The New York Review of Books, 51:3
(February 26, 2004)
-
The Semmelweis Society, an organization dedicated to protecting
physicians from "sham peer review"
-
Semmelweis's first post-stamp, Hungary, 1932
-
Pulse-Project Audio Lecture: Benedek Varga on “The Myth and Cult of
Ignaz Semmelweis: Constructing History of Science during the 20th
Century”

|
|
|
1)
scrivi
le parole inglesi dentro la
striscia gialla
2)
seleziona il testo
3)
clicca "Ascolta il testo"
DA INGLESE A ITALIANO
Inserire
nella casella Traduci la parola
INGLESE e cliccare
Go.
DA ITALIANO A INGLESE
Impostare INGLESE anziché italiano e
ripetere la procedura descritta.
|
|